- HOME
- VENUE
- RSVP
- REGISTRY
- CONTACT
- Fruit of the yew lyrics
- Free commercial pirate fonts
- Cheat for rom hack pokemon tree of time
- 1996 indy 440
- How to do a shutdown timer windows 10
- Eminem discography drive
- Raaz reboot online
- Karnan tamil movie full sivaji
- Fortnite cheats unknowncheats
- Alesis q49 keyboard how do dis
- Propellerhead recycle v 2-2 crack
- What is titan quest anniversary edition
- Ipos 5 kasir
- Kaspersky antivirus versus internet security
- Riane eisler chalice and the blade pdf
- The spongebob squarepants movie 2004 cast
- Fallout 4 cait
- Unison league hack no survey
- Anno 1701 patch 1-04 us
- Warzone resurrection rulebook
- Reflector 2 iphone
- Rapt with attention
- Ossa motorcycle logo
- Backcalculation of hiv infection rates
- How to use advanced file organizer
- How to install transmission filter 1998 s10
- Rap file psn stuff
- Lease instacode

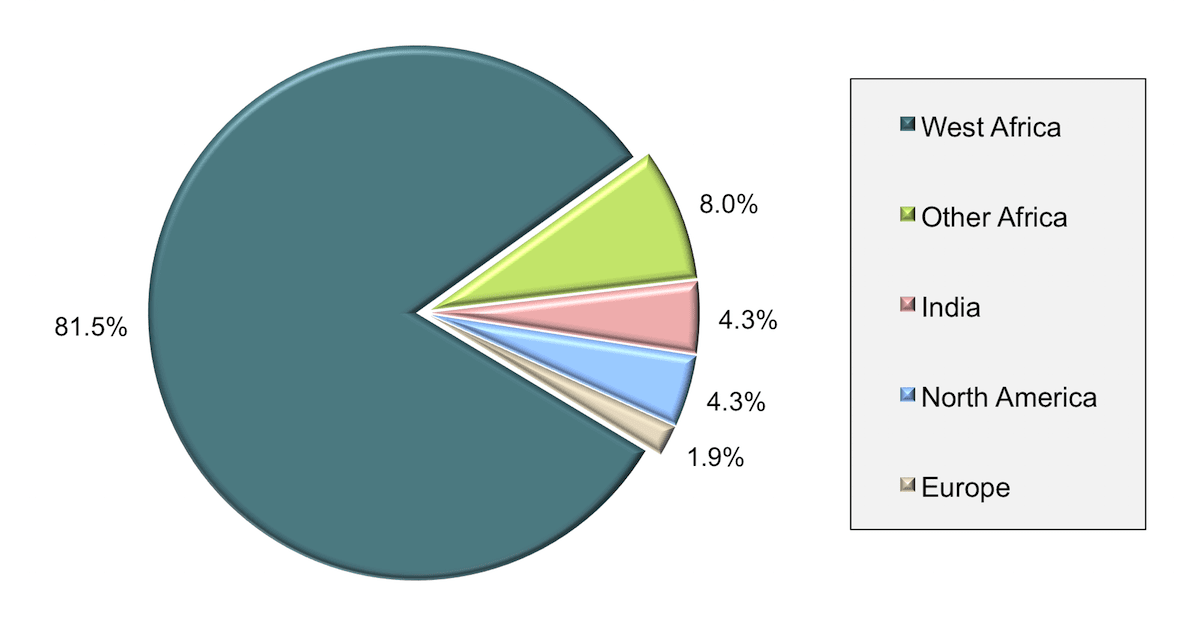
The data showed that vaccination rates were highest in the United States (72%), Peru (69%) and Brazil (63%) and lowest in South Africa (18%), Uganda (3%), and Haiti (0%).Īccording to the study, among the overall REPRIEVE population, people were more likely to be vaccinated if they came from high-income GBD super-region countries were white, male, older aged and had a longer duration of ART and had higher BMI percentages and higher cardiovascular risk.
#Backcalculation of hiv infection rates trial
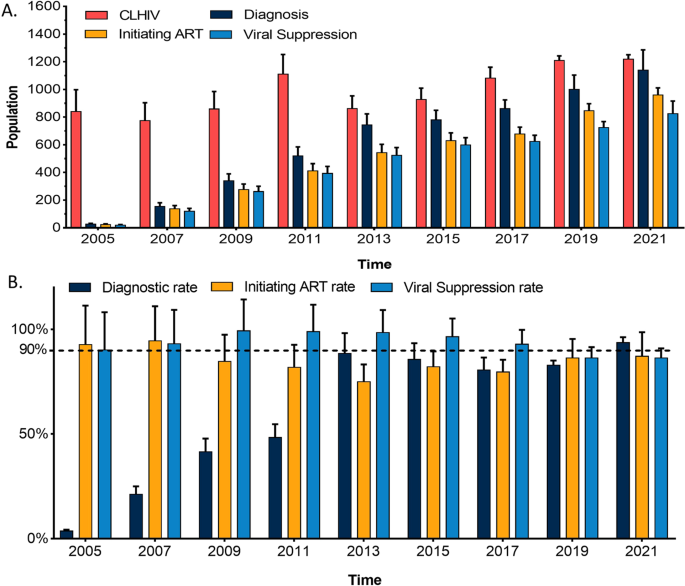
“Thus,” Grinspoon said, “it is critical that people with HIV, representing a vulnerable and immunocompromised population, be vaccinated for COVID-19” - something the NIH has also emphasized in its recommendations.įor their study, Grinspoon and colleagues sought to assess vaccination rates and specific characteristics associated with vaccination in this population by using data from the Randomized Trial to Prevent Vascular Events in HIV (REPRIEVE) a study of people with HIV that is being conducted in 11 countries in both high- and low-income global burden of disease (GBD) regions.Īccording to the study, vaccination rates among REPRIEVE participants were similar to those of the general populations in different countries and GBD regions, although Grinspoon said they found that there were “highly significant differences” in vaccination rates within these regions and countries.įor example, the study showed that although the collective vaccination rate among REPRIEVE participants through the end of July 2021 was 55%, vaccination rates were highest in high-income “super-regions” (71%), followed by Latin America and the Caribbean (59%), South Asia (49%), Southeast/East Asia (41%) and Sub-Saharan Africa (18%).įurther assessment showed that country-specific rates within these regions varied “dramatically,” according to Grinspoon. Although the models are computationally intensive, they provide useful information about seroincidence trends in different age groups.“Data have shown that people with HIV have increased COVID-19 morbidity and mortality,” Steven Grinspoon, MD, professor of medicine at Harvard Medical School and director of the Nutrition Obesity Research Center at Harvard, told Healio. Quantitative estimates were sensitive to the assumed incubation distribution, but the trend toward younger age at HIV infection was apparent using several models of the incubation distribution. However, persons under age 25 years have accounted for an increasing proportion of new HIV infections as the epidemic has progressed. Estimated infection incidence for the entire population declined from peak levels seen in the mid-1980s. The method is applied to AIDS incidence data for the United States population. As in previous applications, the incubation distributions also change over time to accommodate treatment effects and the 1987 revision of the surveillance definition.
The effect of age on progression is estimated from a joint analysis of natural history data from several cohort studies of gay and bisexual men.

In this new approach, the incubation distributions used to backcalculate HIV infection rates depend on the age at HIV infection, because younger age is associated with slower progression. The approach is flexible and allows the distribution of age at HIV infection to change over time. This paper extends the use of backcalculation to estimate past incidence of HIV infection in different age groups from age-specific counts of AIDS incidence.